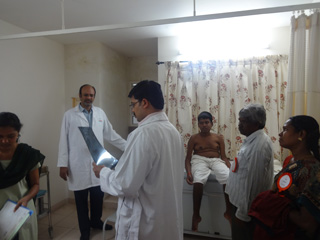
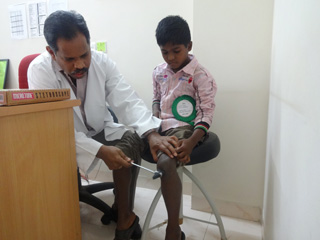
Multidisciplinary Care
Our children affected by DMD need the right diagnosis and special professional care and medical interventions as per global recommendations. It is no longer appropriate to look on DMD as a condition that is inevitably fatal in childhood as the majority can now be expected to reach adulthood with proper care and love. The experts stress that the best management of DMD requires a multidisciplinary approach, with the input of specialists from different areas of care and intervention. An appropriate multi-disciplinary approach for management of these children includes the services of many clinical specialist doctors, lab facilities and specialized equipment like spirometer, Echo cardiogram and Electro cardiogram machines, care givers and rehab specialists.
With the release of the final recommendations from Centre for disease control (CDC, USA) and Treat-NMD on Standards of care for DMD affected children, we have been conducting Multidisciplinary care camps for this purpose.
1. Diagnosis and Management of Duchenne Muscular Dystrophy – part I
2. Diagnosis and Management of Duchenne Muscular Dystrophy – part II
MDCRC handles children in five stages, Presymptomatic, Early ambulatory, late ambulatory, early non-ambulatory and late non-ambulatory. In these clinics, the parents register and give their consent for the examination. This is followed by lab investigations, ECG, X-Ray chest & Spine, Pulmonary Function Tests and clinical examination by the specialist panel of doctors with appropriate advice as per international guidelines with the expertise of the doctors for our Indian children.
Complete team with Paediatricians, Neurologists, Orthopedicians, Rehab specialists, Physiatrists, Pulmonologists, GI, Nutrition and the Diagnostic team has been formed. Evaluation forms were prepared by the team as per CDC USA & Treat NMD International Guidelines. MD Care camps are conducted on Saturdays at MDCRC.
The Multidisciplinary Approach involves
Pediatrics
The pediatrician is concerned with basic changes that are noticed in the children. The Pediatrician records the medical history of the child from birth including details of delivery and immunization schedules, dietary habits and family history. The details regarding Behavioral and attitudinal changes, motor development, delay in development of neurological mile stones are recorded. In addition, the onset of symptoms related to DMD, progression of weakness, investigations done so far and the treatment taken so far are elicited. The pediatrician does a general physical examination and records the vital signs – Heart Rate, Blood Pressure, Respiratory Rate, Oxygen saturation rate (SpO2), Height and weight.
Physiotherapy
Physiotherapists are concerned with enabling children to reach their maximum physical potential. The physiotherapists evaluate the muscle strength including the measurements of Length, Circumference, and Girth. They identify the primary changes in the myology of children. Their aim is to minimize the development of contractures and deformity by developing a programme of stretches and exercises where appropriate, anticipate and minimize other secondary complications of a physical nature, monitor respiratory function and advise on techniques to assist with breathing exercises and methods of clearing secretion, proper seating and positioning to prevent pressure ulcers.
The key contact for management of joint contractures is your physiotherapist. . Stretching should be performed at least 4-6 times each week and should become part of the daily routine.Effective stretching to counteract development of contractures may require different techniques which your physiotherapist will show you, including stretching, splinting and standing devices.
Neurology
Neurologist is concerned with enabling the physical potential of neurology to maximize the preventions from secondary complications. The main evaluation is for muscle strength and tone. They assesses the Stage of the disease, Risk factors for side effects GCs, Choice of regime, Side effects monitoring and prophylaxis, activities of daily living and go for complete clinical evaluation. The neurologist also measures the time it takes for the child to do certain activities such as the time to get up off the floor, time to walk a certain distance, and time to climb several steps. This gives important information on how the condition is changing and how it is responding to treatment. The Doctor will also asses Motor Functioning Scales. During the ambulatory stage of the child (while the child is still walking), the neurologist will recommend steroids intake. Steroids (also called glucocorticoids or corticosteroids) are the only drugs known to slow the decline in muscle strength and motor function in DMD. The goal of steroid use is to help the child walk independently for longer to allow enhanced participation and to later minimize breathing, heart and orthopedic problems. They can also reduce the risk of scoliosis (curvature of the spine). The Neurologist will prevent and manage the side-effects of the steroids during subsequent visits.
Orthopedics
Orthopedicians are concerned with the alignments of bones in their anatomical positions to prevent contractures, deformities, bone health management, long bone fracture management and stress fractures which decline the status of the child. They assess the presence of contractures, grades of deformities, gait pattern if the child is ambulant, sitting and standing balance and the assessment of spine. Spinal care should include monitoring for scoliosis. This is done by clinical observation throughout the ambulatory phase .Surgery can be offered in some situations in an effort to prolong the period of walking. The Orthopedician will recommend the necessary orthotic appliances like splints and braces, knee-foot orthoses, ankle-foot orthoses, wheelchairs and surgical correction of deformities if needed.
Cardiology
Cardiologists assess the cardiac status by physical examination, Electro cardiogram and Echocardiography as per international guidelines for DMD children. Patients should be routinely monitored in early childhood with a complete cardiac evaluation at least every other year. Once the child becomes 10 years of age, yearly cardiac evaluation is compulsory. There will be an increase of cardiac problems with age and they may require intervention even when they are non-symptomatic. The cardiologist will monitor and treat abnormalities of cardiac rhythm. If non-invasive cardiac tests show abnormalities, increased surveillance will be done, at least every six months, and drug treatment will be initiated. The cardiologist will evaluate and suggest treatments according the condition with special focus on children undergoing steroid treatment.
Pulmonology
The Pulmonologist will assess the functional capacity of the lungs with a Pulmonary Function Test. The functional capacity is further assessed using Pulse-Oximetry and Chest- X Ray. Blood investigations may also be done. Respiratory problems are not that common in ambulatory children. However, as the children lose the independence of walking, breathing muscles become affected. The children have an increased risk of infections. For this, the pulmonologist will evaluate past-history of immunizations and may recommend pneumococcal vaccines to prevent infections. Pulmonologist will advise on the required respiratory exercises, need for supplemental oxygen, ventilation assist devices and protection against respiratory infection. As DMD progresses, assistance may be needed for the child to cough and with time support may be needed for breathing. The pulmonologist will proactively prescribe the necessary interventions such as ventilators depending on the requirement of each child.
GI & Nutrition
Children with DMD often require vitamin and mineral supplements to maintain bone density and general health. Maintaining proper diet and nutrition is very important to prevent cardiac problems and general health of the child. The dietician will assess if the child is over-weight or under-weight. Children undergoing steroid therapy may gain excess weight and the nutritionist plays a major role in controlling it. In children in advanced stages of the disease, the dietician will assess if there is any problems of swallowing with the help of X-Rays. The nutritionist will recommend medications to help the child deal with common complaints such as constipation and heart-burns.